In the fall of 2020, Linda first realized she had an organ prolapse. These are extremely common, with a staggering 50% of women over the age of 50 diagnosed with a prolapse issue. And yet, it is a health concern that is rarely discussed. People living with prolapse often experience embarrassment and shame - and don't seek treatment.
Prolapse occurs when a person’s internal organs shift and are pushed into the vaginal space and opening. This can include the rectum, bladder, or uterus. With so few people talking about prolapse, it’s easy to imagine how frightening this experience could be. However, Linda was unphased. As a veteran Registered Nurse, she knew what was happening. “When I had to strain for a bowel movement, something would stick out. Straining at all, or standing for too long would make it worse. I knew it was a prolapse, so I was comfortable pushing it back in with clean hands,” says Linda.
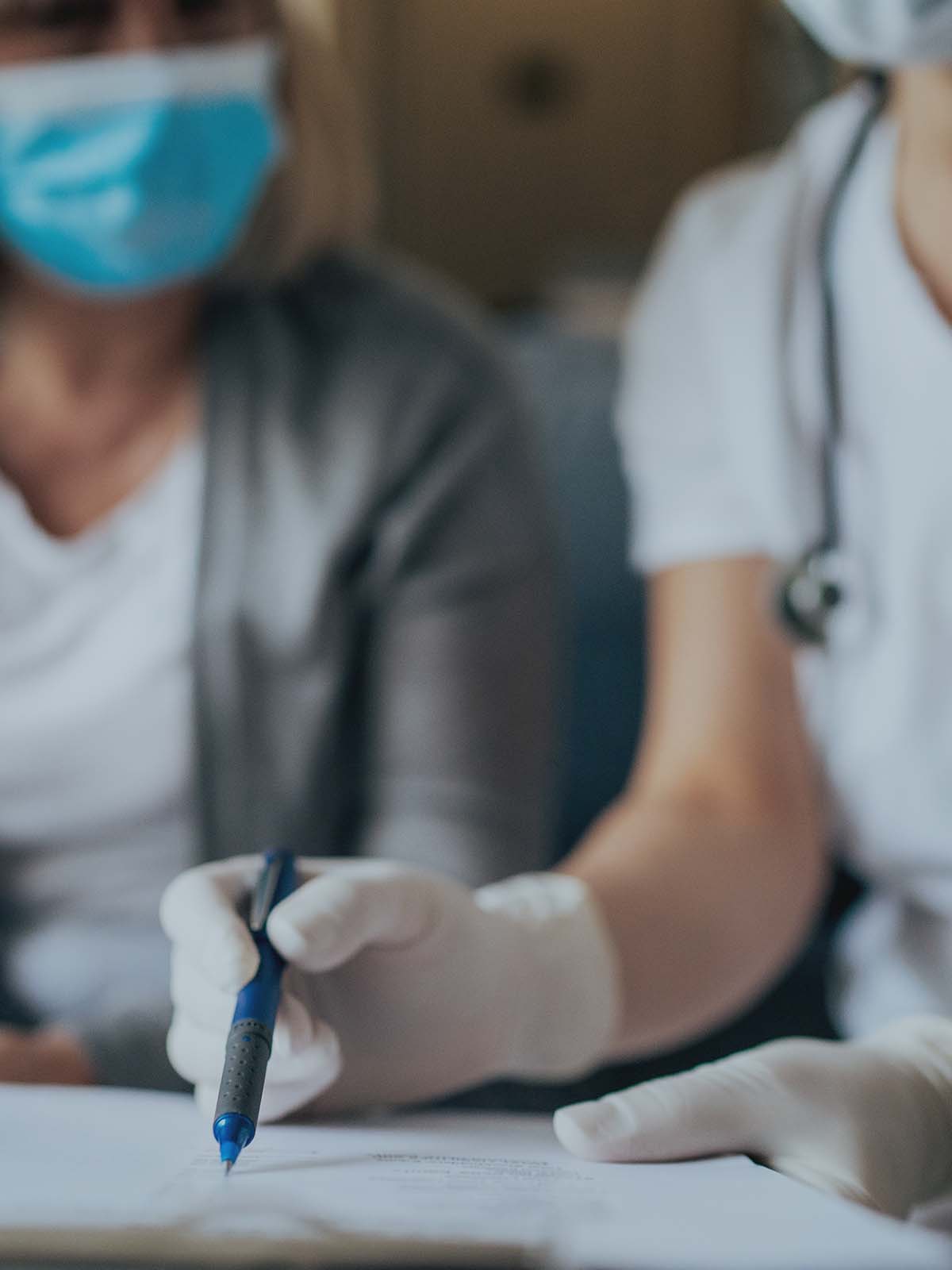
But the issue progressively got worse, so Linda’s family doctor referred her to a pelvic floor physiotherapist. The exercises were extremely helpful, but there was still room for improvement. Linda knew she wanted to speak to a specialist and wanted only the most knowledgeable and experienced health care provider. So when her physiotherapist recommended Dr. Colleen McDermott, a Urogynecologist at Mount Sinai Hospital and the President of the Canadian Society for Pelvic Medicine, Linda knew she had to get an appointment.
“Prolapse is multifactorial and extremely common. It affects 50% of all women over the age of 50,” explains Dr. McDermott. “Non-modifiable risk factors include advancing age, menopause/estrogen deficiency, race, connective tissue disorders, chronic diseases, and patients with some neural issues. Other risk factors include being overweight, having had vaginal births of children, smoking, and chronic constipation.” With so many risk factors, the number of women living with prolapse isn’t surprising. But that doesn't make it any less challenging to relieve. And while there are several treatment options, each comes with its own complications. For Linda a pessary seemed like a good starting point.
The conversation around pelvic floor health has to be initiated and mature women's health has to be made a priority.